


Stable sugars ARE the goal. Always. If a snack helps you feel better and keeps your blood sugar stable, that’s a win.
But here’s the nuance (and it matters in gestational diabetes): a snack in the middle of the night can make your morning number look “perfect”… while masking your true fasting baseline.
This post is specifically about gestational diabetes night snacks (snacks eaten during the night, like 2–4am) — not gestational diabetes bedtime snacks (a bedtime snack eaten before sleep).
Bedtime snack (before sleep): often helpful for many pregnant women. It can support stable blood sugar levels overnight. More on this topic in our Bedtime Snacks for Gestational Diabetes post.
Night snacks (middle of the night): break the fasting window and change what your morning test actually measures.
So yes: blood sugar levels stable is the goal — but we still want a true fasting number when we’re looking at fasting blood glucose levels.
Overnight, your liver releases glucose to keep you going while you’re not eating.
In gestational diabetes, fasting highs often happen because placental hormones (like hPL) increase insulin resistance, and your liver “dumps” more glucose overnight. That’s why fasting is the most hormonal number.
When you eat gestational diabetes night snacks, you can temporarily suppress that liver glucose release — which may help your blood sugar readings look better in the morning.
But it doesn’t fix the underlying insulin resistance.
Example:
Your true fasting baseline might be 105 mg/dL.
You eat a night snack and wake up at 90 mg/dL.
Your blood glucose looks like it’s in a healthy range… but your baseline is still running high.
That matters because an elevated fasting baseline is associated with:
poorer post-meal control later
higher risk of macrosomia / larger baby
higher likelihood you’ll need intervention later
In other words: night snacks can make it easier to miss the moment when your body needs more support (meds/insulin adjustments).
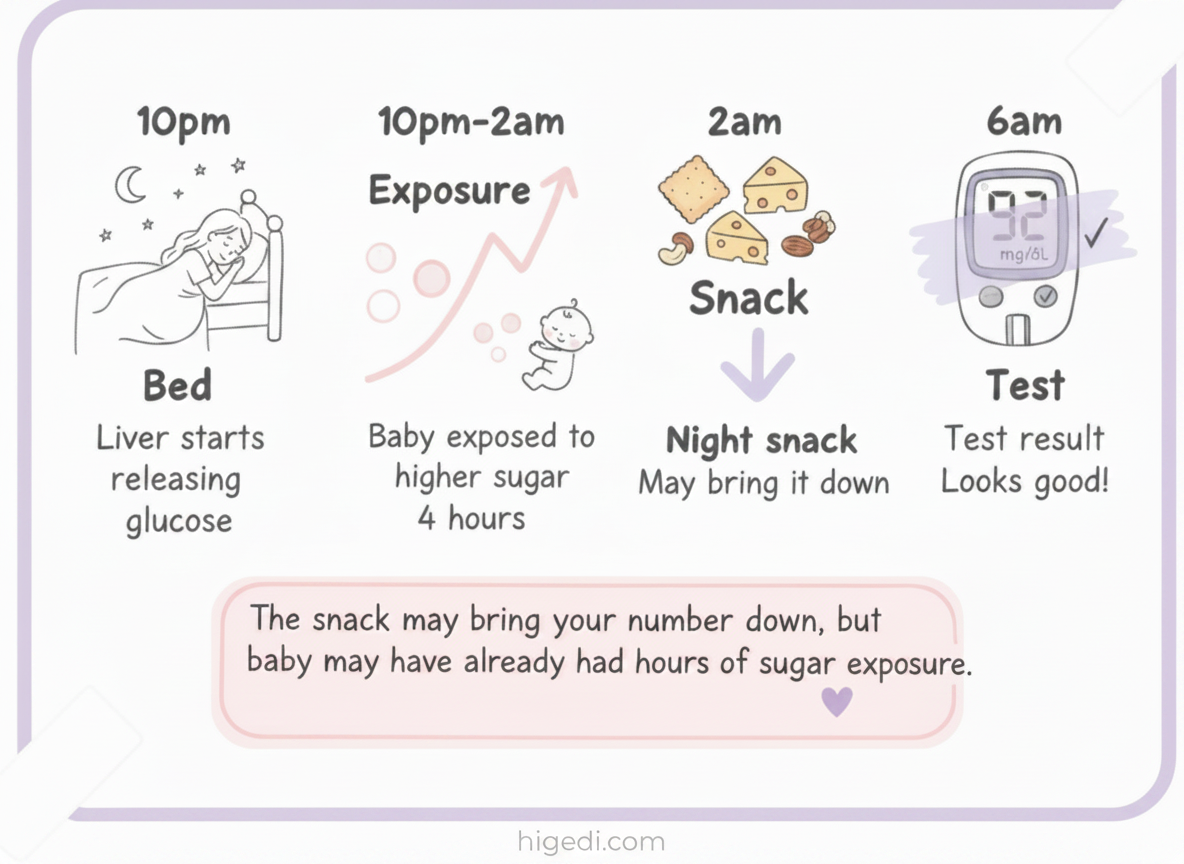
Your night snack may bring your number down. That's possible. But it doesn't change what happened in those hours before you ate it.
If your liver started dumping glucose at 10pm and you didn't eat until 2am, baby was exposed to higher sugar for those 4 hours. Even if the snack helps, it can't rewind that. It just creates a mask on your 6am test.
So when you see that nice morning number after a snack, you're seeing a masked picture. Your provider can't tell from that number alone whether baby got a 2-hour sugar bath or a 4-hour one — or whether the underlying liver dump is getting worse as pregnancy progresses.
That's why seeing true fasting number (without the snack) matters: it helps your team understand what's actually happening overnight, so they can decide if baby needs protection (like insulin) rather than just a mask.
Night eating every day is exhausting. And as pregnancy progresses, what “works” at 28 weeks may stop working at 34–36 weeks.
A true fasting number (without night eating) helps your team see trends and adjust proactively — especially if you’re following a personalized meal plan or using insulin.
Fasting baseline is one of the strongest predictors of adverse outcomes in gestational diabetes — even if daytime numbers look great.
Think of it like this: it’s the difference between checking your weight fasted vs. after a big meal. Both are “real,” but fasting shows the baseline.
When fasting runs high overnight, baby is exposed to higher glucose for hours. Baby responds by making more insulin, which can contribute to extra growth.
That’s why your care team cares about unmasked fasting numbers — even if a snack makes them look perfect.
Some commonly cited risk stats:
About 15–30% of gestational diabetes babies are macrosomic (>9 lbs) (Source)
Shoulder dystocia happens in 5–16% of macrosomic babies (vs <1% normal-weight) (Source)
Bottom line: it’s better to catch a rising fasting baseline now than find out at delivery that baby is very large and delivery gets complicated.
If you’re currently doing night snacks, you’re not “cheating” or “failing.” You’re coping.
But if you suspect night snacks are masking your baseline, consider:
Tell your care team you’re eating overnight (this is important context for interpreting your numbers)
Ask what they want you to do for testing (some teams want a true 8–10 hour fast for a few nights to assess baseline)
If you wake up with low blood sugar symptoms, treat it — safety first — and then talk to your provider about adjusting meds/food
And yes: you can still do a bedtime snack before sleep if that helps you feel steady. Just try to avoid eating in the middle of the night unless it’s medically necessary.
If you need help lowering fasting (without in the middle of the night snacks), this How to Lower Fasting Blood Sugar guide can help.
If you’re early in gestational diabetes and this feels like a lot, start here.
And remember: managing gestational diabetes is not about perfection. It’s about patterns, support, and getting you and baby safely to the finish line.
1. Is a bedtime snack the same as a night snack?
No. A bedtime snack is eaten before sleep. Gestational diabetes night snacks are eaten in the middle of the night and break the fasting window.
2. If my blood sugar is stable after a night snack, why does fasting still matter?
Because fasting shows your baseline. Night snacks can suppress your liver’s overnight glucose production temporarily and mask rising insulin resistance.
3. If my fasting is high, should I eat in the middle of the night to "bring it down"?
No — that's the masking problem. A night snack can make your morning number look better without improving the underlying fasting physiology.
4. What's the "best" night snack for gestational diabetes?
There isn't one — because in theory, you shouldn't be eating anything at night if you want a true fasting number. The whole point is to get an unmasked baseline. If you must eat (safety concerns, true low blood sugar, medical reasons), tell your team so they can interpret your data correctly and adjust your plan.
5. Can I still have a bedtime snack?
Yes. Gestational diabetes bedtime snacks (before sleep) are a separate thing and are often part of a balanced plan — especially if they help keep blood sugar levels stable overnight.
6. I'm hungry at night — does that mean my bedtime snack is wrong?
Not always, but it can mean your bedtime snack isn't keeping you satisfied. It can also mean you're under-eating during the day, your dinner was too light, or pregnancy discomfort/stress is waking you up. If it's happening often, bring it up — your care team can help adjust your plan.
7. What if I'm on insulin and I'm scared of going low overnight?
Valid fear. Don't guess alone. Ask your team what bedtime snack they recommend with your dose, and what to do if you wake up feeling low. If you have symptoms of low blood sugar, treat it.
8. What if I wake up truly low?
Treat the low. Then tell your care team — frequent overnight lows may mean meds or your plan needs adjusting.
Disclaimer: This post is not medical advice. Please talk to your healthcare provider about your specific situation and follow their treatment plan.
Get a Free 20-Day Shopping List